Femur Fracture Physical Therapy Protocol
This protocol details rehabilitation post-femoral fracture, utilizing a multidisciplinary approach with surgeons and therapists.
Early mobilization, tailored exercises, and progressive weight-bearing are key components for optimal recovery and functional restoration.
Femur fractures represent significant orthopedic injuries requiring comprehensive rehabilitation to restore optimal function. This physical therapy protocol outlines a phased approach to recovery following a femur fracture, whether stabilized with intramedullary nailing or other fixation methods. The goal is to guide clinicians and patients through a structured program, maximizing strength, range of motion, and ultimately, a return to pre-injury activity levels.
Successful rehabilitation necessitates a collaborative effort between orthopedic surgeons, physical therapists, and the patient. Early mobilization, as highlighted in recent studies, is crucial. This protocol emphasizes progressive weight-bearing, proprioceptive training, and individualized exercise regimens. Consideration of specific fracture types – such as subtrochanteric or comminuted distal femur fractures – is also vital, as these may necessitate modifications to the standard progression. Post-implant removal rehabilitation also requires specific attention.
Understanding Femur Fractures
Femur fractures are breaks in the thigh bone, ranging in severity from stable hairline fractures to complex, comminuted breaks. These injuries commonly result from high-energy trauma, such as falls or motor vehicle accidents, but can also occur in individuals with weakened bones. Fracture location significantly impacts treatment and rehabilitation; proximal femur fractures (near the hip) differ greatly from distal femur fractures (near the knee), and subtrochanteric fractures present unique challenges.
Fixation methods, like intramedullary nailing, are frequently employed to stabilize the fracture. Understanding the specific fracture pattern and chosen fixation technique is crucial for tailoring the rehabilitation program. Comminuted fractures, involving multiple bone fragments, often require a more prolonged and cautious approach. Post-surgical considerations, including potential implant removal, also influence the rehabilitation timeline and goals, demanding a multidisciplinary approach.

Phase 1: Immediate Post-Operative (Weeks 0-4)
Initial focus is on pain and edema control, gentle range of motion, and weight-bearing as tolerated, progressing from assistive devices to independent ambulation.
Weight Bearing Protocol
Initial weight-bearing status is crucial and dictated by fracture stability and surgical fixation method. Typically, in the immediate post-operative phase (Weeks 0-4), patients begin with weight-bearing as tolerated (WBAT) utilizing assistive devices like walkers or crutches.
Progression occurs gradually, monitored by the physical therapist and surgeon. The goal is to transition from toe-touch weight-bearing to partial weight-bearing (PWB), then to weight-bearing as tolerated (WBAT), and ultimately to full weight-bearing (FWB).
This progression is dependent on radiographic evidence of healing and the patient’s pain levels. Intramedullary nailing often allows for earlier weight-bearing compared to other fixation methods. Careful assessment of gait and biomechanics is essential throughout the process, ensuring proper loading and minimizing stress on the fracture site. The timeline for achieving FWB varies significantly based on individual factors and fracture characteristics.
Range of Motion Exercises
Early initiation of range of motion (ROM) exercises is vital to prevent stiffness and maintain joint mobility following a femur fracture. In Phase 1 (Weeks 0-4), focus on active, active-assisted, and passive ROM exercises for the hip, knee, and ankle. Gentle ankle pumps and knee bends are initiated immediately to reduce swelling and improve circulation.
Hip ROM is progressed cautiously, avoiding excessive flexion or rotation that could compromise the fracture site. Emphasis is placed on achieving full knee extension. As pain subsides, the range of motion is gradually increased.
Proprioceptive training is incorporated to enhance joint awareness and neuromuscular control. These exercises help restore normal movement patterns and prepare the patient for more advanced rehabilitation. Consistent, gentle ROM exercises are crucial for optimizing functional outcomes and preventing long-term complications.
Pain Management Strategies
Effective pain management is paramount throughout the femur fracture rehabilitation process. Initially, pain control relies on prescribed analgesics, as directed by the orthopedic surgeon. Physical therapy interventions complement pharmacological approaches, focusing on reducing pain and improving function.
Modalities such as ice and elevation are employed to minimize swelling and alleviate discomfort. Gentle range of motion exercises, performed within a pain-free range, help to restore joint mobility and reduce muscle spasms.
Patient education regarding pain management techniques, including proper positioning and activity modification, is crucial. As rehabilitation progresses, the focus shifts towards active pain management strategies, such as strengthening exercises and proprioceptive training, to enhance functional capacity and reduce reliance on medication.
Edema Control
Post-operative edema is a common occurrence following femur fracture repair, significantly impacting comfort and hindering rehabilitation progress. Early and consistent edema control is therefore a critical component of the physical therapy protocol. Elevation of the affected limb above the heart is a foundational strategy, promoting venous return and reducing fluid accumulation.
Compression bandages are applied to minimize swelling and provide support. Gentle ankle pumps and active muscle contractions, performed regularly, aid in lymphatic drainage and circulation.
Monitoring the circumference of the leg provides objective data to track edema reduction. Patients are educated on self-management techniques, including proper bandaging and activity modification to prevent exacerbation of swelling. Consistent implementation of these strategies facilitates improved comfort, enhanced range of motion, and accelerated recovery.

Phase 2: Early Rehabilitation (Weeks 4-8)
This phase focuses on progressive weight-bearing, strengthening quadriceps, hamstrings, and glutes, alongside proprioceptive training to regain stability and function.
Progressive Weight Bearing
Weight-bearing progression is crucial during weeks 4-8, carefully monitored by the physical therapist. Initially, patients typically transition from non-weight-bearing to toe-touch weight-bearing, utilizing assistive devices like walkers or crutches. As pain subsides and radiographic evidence of healing progresses, partial weight-bearing is introduced, gradually increasing the percentage of body weight supported on the affected limb.
The goal is to achieve full weight-bearing by the end of this phase, but this is individualized based on fracture stability and patient tolerance. Regular assessment of pain levels, swelling, and gait pattern guides the progression. Emphasis is placed on proper form and avoiding compensatory movements. Transitioning from crutches to a cane, and ultimately to independent ambulation, is a key milestone. The protocol, as outlined by Gross (2026), emphasizes a tailored approach, adapting to individual needs and healing rates.
Strengthening Exercises ⎯ Quadriceps
Quadriceps strengthening is paramount in weeks 4-8, addressing significant muscle atrophy post-injury and immobilization. Initial exercises focus on isometric contractions – quad sets performed by tightening the thigh muscles without joint movement – to activate the muscle without stressing the fracture site.
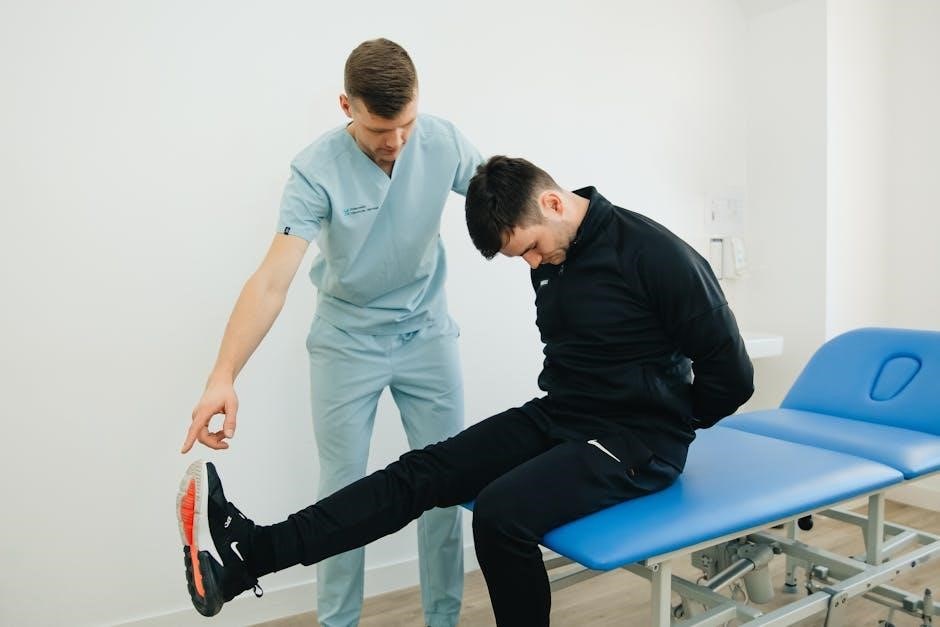
Progressing to short-arc quads, performed with a small range of motion, builds strength and endurance. Straight leg raises, in various planes, further challenge the quadriceps. As weight-bearing increases, closed-chain exercises like wall slides and mini-squats are incorporated.
Resistance is gradually added using ankle weights or resistance bands. The aim is to restore full quadriceps strength, essential for gait normalization and functional activities. Consistent adherence to the prescribed exercise regimen, guided by a physical therapist, is vital for optimal outcomes.
Strengthening Exercises ⏤ Hamstrings & Glutes
Hamstring and gluteal strengthening is crucial for hip extension, stabilization, and overall lower extremity function, typically initiated during weeks 4-8 alongside quadriceps work. Initial exercises include gluteal sets – squeezing the buttocks muscles – and hamstring sets, activating these muscle groups isometrically.
Bridging exercises, starting with both legs and progressing to single-leg bridges, effectively target the glutes and hamstrings. Prone hip extensions and hamstring curls with resistance bands provide additional strengthening.
As strength improves, functional exercises like step-ups and lunges (when appropriate based on fracture healing) are introduced. Strengthening these posterior chain muscles is vital for restoring a normal gait pattern and preventing compensatory movements. Consistent exercise, guided by a therapist, is key.
Proprioceptive Training
Proprioception, or the body’s awareness of its position in space, is often impaired following a femur fracture and subsequent surgery, necessitating targeted training. This training typically begins in Phase 2 (weeks 4-8) and continues throughout rehabilitation. Initial exercises involve weight shifting in various directions while maintaining balance, often starting with a stable surface.
Single-leg stance, initially with support and progressing to unsupported, challenges balance and proprioceptive abilities. Utilizing unstable surfaces like foam pads or wobble boards further enhances these skills.
Exercises incorporating perturbations – gentle pushes or pulls – help the patient react and regain control. Proprioceptive training is essential for restoring normal gait, preventing falls, and optimizing functional recovery, particularly after implant removal.

Phase 3: Intermediate Rehabilitation (Weeks 8-12)
This phase focuses on building strength and normalizing movement patterns, progressing towards functional activities with advanced exercises and balance work.
Advanced Strengthening Exercises
During this phase, strengthening progresses beyond basic exercises to challenge the recovering limb more significantly; Focus shifts to closed-chain exercises, mimicking real-life movements and enhancing functional strength. Examples include leg presses, utilizing increasing resistance, and step-ups onto varying heights to build quadriceps and gluteal strength.
Hamstring curls and hip abduction/adduction exercises with resistance bands further contribute to overall lower extremity stability. Single-leg stance exercises, progressing from stable to unstable surfaces (foam pads, wobble boards), are crucial for improving balance and proprioception. Core strengthening exercises, such as planks and bridges, are integrated to provide a stable base for lower extremity function.
It’s vital to monitor patient response and adjust resistance accordingly, preventing overexertion and ensuring proper form. The goal is to achieve near-normal strength levels, preparing the patient for more demanding functional activities.
Gait Training ⏤ Normalization
The focus now transitions to refining gait mechanics, aiming for a natural and efficient walking pattern. This involves addressing any remaining gait deviations, such as limping or altered step length. Exercises include focused attention on heel strike, toe-off, and symmetrical arm swing.
Patients practice walking over varied terrains – inclines, declines, and uneven surfaces – to challenge balance and adaptability. Mirror feedback can be utilized to provide visual cues for correcting gait abnormalities. Emphasis is placed on increasing walking speed and endurance, gradually reducing assistive device reliance.

Proprioceptive exercises continue to play a role, enhancing awareness of limb position during gait. Regular assessment of gait parameters – step length, cadence, and joint angles – guides progression. The ultimate goal is independent ambulation with a normal gait pattern, minimizing compensatory movements and maximizing functional mobility.
Balance and Coordination Exercises
Restoring dynamic balance and coordination is crucial for functional independence following a femur fracture. Initial exercises involve static balance activities, such as single-leg stance with varying levels of support, progressing to dynamic challenges. These include tandem stance, reaching activities in multiple directions, and perturbation training to challenge reactive balance control.
Coordination drills, like walking with head turns or performing upper extremity movements while maintaining balance, are incorporated. Use of unstable surfaces – foam pads or wobble boards – further enhances proprioception and neuromuscular control.
Functional tasks, such as stepping over obstacles and navigating around furniture, are practiced to simulate real-life scenarios. The aim is to improve anticipatory and reactive postural adjustments, reducing the risk of falls and enhancing overall stability during ambulation and daily activities.

Phase 4: Advanced Rehabilitation & Return to Function (Weeks 12+)
This phase focuses on regaining full function, incorporating sport-specific training if applicable, and progressing to complex movements like squats and lunges.
Functional Exercises ⏤ Stair Climbing
Stair climbing is a crucial functional exercise progressively introduced to assess and improve lower extremity strength, balance, and coordination following a femur fracture. Initially, patients begin with assisted stair climbing, utilizing handrails for support and focusing on controlled ascents and descents. The therapist monitors for compensatory patterns, such as excessive trunk lean or hip hiking, providing cues to maintain proper biomechanics.
As strength improves, the level of assistance is gradually reduced, progressing to independent stair climbing with alternating reciprocal patterns. Emphasis is placed on full hip and knee extension during each step, ensuring adequate quadriceps and gluteal muscle activation. The height of the stairs can be modified to increase the challenge.
Progression includes negotiating varied stair surfaces and incorporating stair climbing into functional tasks, such as carrying light objects. The goal is to achieve independent, safe, and efficient stair climbing, replicating real-life demands and facilitating a return to prior functional levels.
Functional Exercises ⎯ Squats & Lunges
Squats and lunges are essential functional exercises designed to restore lower extremity strength, power, and functional movement patterns after a femur fracture. Initially, patients begin with partial-range squats, focusing on maintaining proper form – a neutral spine, engaged core, and controlled descent. Assistance may be provided using a chair or support for balance.
As strength improves, the range of motion is gradually increased, progressing towards full squats. Lunges are introduced, starting with short steps and emphasizing controlled knee tracking over the ankle. Both exercises challenge quadriceps, hamstrings, and gluteal muscles, crucial for functional activities.
Progression involves adding resistance using weights or resistance bands, and incorporating variations like single-leg squats and walking lunges. The ultimate goal is to achieve independent, pain-free squats and lunges, enabling patients to confidently perform daily activities requiring lower extremity strength and stability.
Sport-Specific Training (If Applicable)
For athletes returning to sport post-femur fracture, a dedicated sport-specific training phase is crucial. This phase builds upon the foundation of strength, power, and functional movement established in previous rehabilitation stages. It involves replicating the demands of the athlete’s specific sport, gradually increasing intensity and complexity.
Training incorporates drills that mimic sport-related movements, such as agility drills, plyometrics, and sport-specific skill practice. Emphasis is placed on proper technique, neuromuscular control, and reactive strength. A progressive overload principle is applied, carefully monitoring the athlete’s response and adjusting the program accordingly.
Return-to-sport criteria must be met, including full, pain-free range of motion, adequate strength and power, and successful completion of functional tests. Collaboration between the physical therapist, physician, and coach is essential to ensure a safe and effective return to competition, minimizing the risk of re-injury.

Specific Fracture Types & Considerations
Fracture location impacts rehabilitation; subtrochanteric, distal, and comminuted fractures require tailored protocols.
Intramedullary nailing rehabilitation necessitates specific post-implant removal considerations for optimal outcomes.

Subtrochanteric Femur Fractures
Subtrochanteric femur fractures (STF), occurring within 5cm of the lesser trochanter, present unique rehabilitation challenges. Initial management focuses on stabilization, often with intramedullary nailing, followed by a carefully progressed weight-bearing protocol. Early phases (Weeks 0-4) emphasize non-weight bearing or touch-down weight bearing to protect the fracture site, coupled with gentle range of motion exercises to maintain joint mobility and prevent stiffness.
As healing progresses (Weeks 4-8), progressive weight-bearing is introduced, guided by radiographic evidence of callus formation. Strengthening exercises targeting the quadriceps, hamstrings, and gluteal muscles are crucial for restoring lower extremity function. Proprioceptive training is initiated to enhance balance and coordination. Later phases (Weeks 8-12+) involve advanced strengthening, gait normalization, and functional exercises, preparing the patient for return to activities. Close monitoring and individualized adjustments are essential due to the potential for delayed union or non-union in STF.
Distal Femur Fractures
Rehabilitation following distal femur fractures, particularly those requiring surgical intervention like intramedullary nailing or external fixation, demands a comprehensive and phased approach. Early mobilization is prioritized, focusing on restoring range of motion and minimizing stiffness. Weight-bearing progression is dictated by fracture stability and healing, starting with protected weight-bearing and advancing as tolerated;
Proprioceptive training plays a vital role in regaining neuromuscular control and balance, addressing deficits often present after immobilization. Tailored exercise regimens target quadriceps, hamstring, and calf muscle strengthening, crucial for functional recovery. Post-implant removal, a specific rehabilitation phase focuses on restoring full range of motion and addressing any residual muscle weakness. A multidisciplinary team – surgeons, physical therapists, and rehabilitation specialists – ensures optimal outcomes, emphasizing individualized care and progressive challenges.
Comminuted Distal Femur Fractures
Managing comminuted distal femur fractures necessitates an extended and meticulously planned rehabilitation protocol. These complex injuries, often requiring surgical intervention, present unique challenges due to significant bone loss and soft tissue damage. Initial phases prioritize pain and edema control, alongside gentle range of motion exercises to prevent stiffness.
Progressive weight-bearing is cautiously implemented, guided by radiographic evidence of healing and clinical assessment. Strengthening exercises, focusing on the quadriceps, hamstrings, and gluteal muscles, are gradually introduced to restore lower extremity function. Proprioceptive training is crucial for regaining balance and coordination. A multidisciplinary approach, integrating orthopedic surgeons and physical therapists, is essential for optimizing recovery and addressing specific patient needs, particularly after implant removal, ensuring a return to pre-injury activity levels.
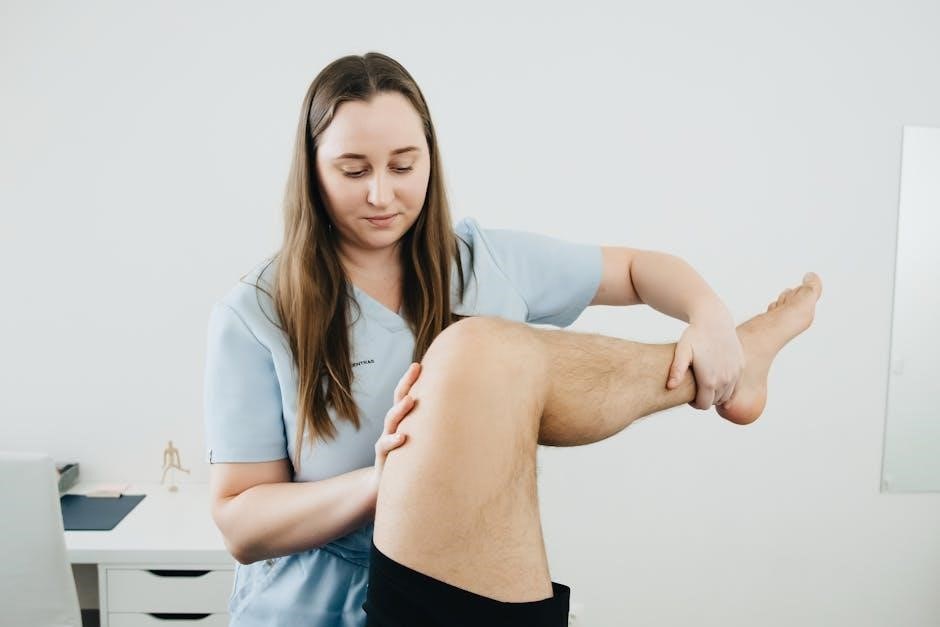
Intramedullary Nailing Rehabilitation
Rehabilitation following intramedullary nailing emphasizes early mobilization, progressive weight-bearing, and tailored exercise regimens to restore function and address post-implant considerations.
Post-Implant Removal Rehabilitation
Following implant removal, a focused rehabilitation program is crucial to address deficits stemming from the previous hardware. This phase necessitates a multidisciplinary approach, integrating orthopedic surgeons, physiotherapists, and rehabilitation specialists to optimize patient outcomes. Emphasis is placed on restoring full range of motion, often hindered by prolonged immobilization or the presence of the implant itself.
Proprioceptive training becomes paramount, as the altered biomechanics during the healing process can impair joint position sense and balance. Tailored exercise regimens are designed to strengthen weakened musculature, particularly the quadriceps, hamstrings, and gluteal muscles, progressively increasing the intensity and complexity of movements.
Gait analysis and retraining are essential to normalize walking patterns, addressing any compensatory strategies developed during the initial phases of recovery. The goal is to achieve symmetrical weight-bearing, efficient stride length, and a smooth, pain-free gait; Individualized programs consider the patient’s specific needs and functional goals, ensuring a comprehensive and effective rehabilitation experience.
Multidisciplinary Approach
Optimal femur fracture rehabilitation demands a collaborative, multidisciplinary approach. This involves close communication and coordinated care between orthopedic surgeons, physical therapists, rehabilitation specialists, and potentially pain management professionals. The surgeon’s expertise guides the overall treatment plan and monitors bone healing, while the physical therapist designs and implements individualized exercise programs.
Rehabilitation specialists contribute by addressing functional limitations and maximizing the patient’s ability to return to daily activities. Pain management strategies, if needed, ensure patient comfort and facilitate participation in therapy. Regular team meetings are vital to discuss patient progress, adjust the rehabilitation plan, and address any emerging challenges.
This integrated approach ensures holistic care, addressing not only the physical aspects of recovery but also the psychological and social factors that can influence outcomes. A unified team effort maximizes the potential for a successful and lasting return to function.
